
I don’t know why it has been so hard for me to sit down and write this post. I have postponed it for +30 weeks (or technically two years) now. I decided not to share our fertility journey in real time for a few reasons. One being because I never thought it would take us as long as it did or that we would end up going down the path we ultimately took. Having two healthy pregnancies and babies before, I was pretty naive about what it would look like for us to get pregnant again. Afterall, it’s worked twice in the past so it should be easy, right?




The second reason I have been so hesitant to share our story is because we DO have two precious, healthy blessings from God that I don’t take for granted for one second. I know so many women are actively trying to get pregnant with their first child, but still struggling after months and years of failed attempts, tens of thousands of dollars spent on failed fertility treatments and quite frankly feeling alone and emotionally drained. I never want our story to come across as seeking sympathy or not being grateful for all our many blessings. Because I am very much aware of how full our life is now and how full it would continue to be if we were not able to have another child. I know our path to getting pregnant is not nearly as challenging and taxing as the journey many women face. So please know this is not coming from a place of seeking sympathy or comparison.
Lastly, I waited to share our journey because it is such an emotional roller coaster each month already. The added pressure of an even larger audience (other than our close friends and family) waiting for pregnancy news each month (after month) sounded daunting and overwhelming. I don’t think there is any ‘right’ way to share whether its’ fertility issues, pregnancy announcement timing, miscarriage or any other challenge we go through as women. I believe it is a personal choice for everyone, and I respect other influencers or individuals for their personal choice, but this was what felt right for us.
I promise this is my last caveat before I get ‘into it’. But I also want to tell you why we are opening up about our journey at all. I personally found that when you are going down such a path of unknowns, when Dr’s are quoting statistics and options, you want to know as much about other people’s experiences as possible to help make an informed decision about your next steps. And also to seek hope in other’s success stories. I found myself reading all the forums online after every ‘treatment’ comparing my faint pregnancy test lines to strangers’ on the internet trying to determine if it was just another false positive from the trigger shot or a true early positive. (If you have ever been in this position, you know what I am talking about!) I hope sharing our story will serve as that life line to someone else going through a similar situation. I also hope in some small way it helps open up the conversation about infertility in general so it doesn’t have to be such taboo topic for those who don’t want it to be.
All that being said, here is a timeline of our path to becoming pregnant with ‘baby sister’ as we are calling her around here. Warning, this will be a long one, but my goal is to answer all your questions from DM’s and to be a resource in any small way to someone else in a similar situation. Grab a cup of coffee and get comfortable because in my eight years of blogging, I think this counts as the longest post EVER!
First, A little Background
For a little background, Fred and I both come from families of three – he is the baby and I am the middle child. Perhaps that has something to do with it, but we always thought we would have three children, as well. And since you always hear about 35 being this (not so) magical number where it gets harder to conceive and carry a healthy pregnancy, my Type A personality thought we would start having kids at 30 and be done before 35. I turned 30 a few months after having Knox and 32 two months after having Andrew. So the original plan was to be 34 for baby #3. (For reference, I turned 36 on Monday.)
Obviously *35* is a very loose number and everyone woman is different. But, for those of you not familiar, a pregnancy that occurs when a person is 35 years or older is known as an advanced maternal age pregnancy. In the medical world, it’s also sometimes known as a “geriatric pregnancy”.
When the time came to start trying to conceive again, we decided to space the next baby a little further apart than Knox and Andrew are (they are 26 months apart). I was honestly still overwhelmed with work and two kids so young in age so Fred and I talked and decided that 2.5 years would be more ideal spacing between Andrew and our last baby. I laugh now at how we thought we had control over any of this. 😉
When did you seek medical help or start to think something may be wrong?
After about six months of trying on our own, I was scheduled for my annual OBGYN appointment. I honestly wasn’t too worried at this point. I knew the statistics that it could take up to a year to conceive for a couple that didn’t have any fertility issues so I still felt patient at this point. However, I did mention our status to my doctor when she asked about our family planning. She suggested we do some routine blood work while I was there just to make sure everything was okay. But since I had no problem getting pregnant before, she was sure everything was fine. Her advice was to continue trying on our own and check back in 4 months if anything still hadn’t happened. I left the doctor that day not thinking much of the bloodwork and was prepared and hopeful to continue trying on our own. A few days later the nurse called me to go over all my numbers, she started by telling me about all the test that looked ‘normal’, but then told me my AMH level came back in what they call the ‘grey area’. My number wasn’t so low that it was impossible to get pregnant on my own, but certainly lower than they like to see for my age. My AMH at 34 was a 1.3 where a typical number for my age is 2.3. So my AMH is more inline for what you would see for a woman in her 40’s. Anything below one and they automatically refer you to a Reproductive Endocrinologist, but since I was in the ‘grey area’ she suggested we continue trying on our own a few more months and then she would refer me after 9 months of TTC (trying to conceive) to a specialist.
For those of you who, like me, aren’t familiar with AMH levels and what it means, here is a little information from google.
“Anti-Müllerian hormone, or AMH, is a protein hormone produced by special cells inside the ovarian follicles. The level of AMH in the blood can help doctors estimate the number of follicles inside the ovaries, and therefore, the woman’s egg count. A typical AMH level for a fertile woman is 1.0–4.0 ng/ml; under 1.0 ng/ml is considered low and indicative of a diminished ovarian reserve.”
After learning about my AMH level and lots of googling, I was starting to get a little concerned. We tried another few months on our own putting us at 8 months of TTC before making an appointment with a fertility doctor.
How did you find the right doctor for you?

I honestly don’t know if I would have gone to a fertility specialist (Reproductive Endocrinologist) before one full year of TTC on our own if it wasn’t for one of my girlfriends who was already a patient. She knew how long we had been trying and she knew about my AMH levels and encouraged me to just go talk to our friend, neighbor and now doctor, Dr. Ryan Steward at Houston Fertility Institute. Dr. Steward also happens to be the Reproductive Endocrinologist my OBGYN refers her patients to so he was the obvious choice for us for multiple reasons. All bias aside since we know him personally, I can’t recommend him or his team enough. It was always easy to get an appointment and to communicate with his team of nurses. We always got timely feedback and thorough instructions after each appointment through their patient portal. It was easy to communicate through message or phone calls and I always felt like Dr. Steward and his team had our personal best interest at heart and were truly invested in our personal care and our fertility journey.
What fertility treatments did you start with?
It was now August 2018 and we had been TTC for 8 months. Fred and I made an appointment to meet with Dr. Steward to talk through our medical history, how long we had been trying on our own, what our options were, etc. We decided to start with more blood work to confirm the previous blood work done at my OB was accurate, a sonogram to see where I was in my cycle and to make sure everything looked okay and to test Fred to make sure everything was okay with him, as well. Everything came back as expected so we ultimately decided to do a Hysteroscopy to rule out that anything was wrong with the shape of my uterus (because I had two preterm labors with the boys due to my water breaking at 34 weeks) and to look for any other abnormalities. During this procedure, they can flush your tubes to clear out any potential blockage and correct any scar tissue or other potential issues that could be causing fertility problems. Again, everything looked perfectly normal so now, other than my AMH level, everything else seemed to be perfectly fine.
September 2018: For our first month of TTC with Dr. Steward (after initial testing and the Hysteroscopy), we decided to start with a monitored cycle on Clomid. From my understanding, this is a pretty common, conservative first step in the process. The monitored cycle is important because your doctor is monitoring your body’s reaction to the medication and because they are testing your hormone levels and watching your progress each step of the way. This is important to find any potential problems that could be causing the infertility in the first place and to make sure you are responding as planned to the medication. I had a great response to the medicine (one mature follicle in my left ovary and three in my right!), but obviously didn’t get pregnant this month. I developed ovarian cysts on both ovaries as a side effect to the Clomid so I was put on birth control to ‘quiet the ovaries’ and wait for the cyst to go away naturally. The most frustrating thing about this is that you have to wait another month before you can try again. The ironic thing about the ups and downs of infertility is that I remember taking a picture of the sonogram screen thinking one of these follicles could be our baby!
October 2018: Ovarian cyst. Had to sit this month out.
November 2018: Once the cyst were gone and my estrodril was back to normal, we could try again. This time I took Letrozole, a drug similar to Clomid, hoping to avoid the cysts this time around. I didn’t respond as well to this medicine in terms of number of follicles (I only had one mature follicle in my right ovary). I traveled with my family to Germany this month and remember going into a Pharmacy to purchase a pregnancy test. I had this idea in my head that I would buy a little German souvenir to take back to Fred to tell him we were pregnant. I didn’t get pregnant this month.
December 2019 : Another cycle of Letrozole, one mature follicle in each ovary -> not pregnant. Each month I would be so optimistic and think this was it! This month I imagined wrapping gifts for the family to open Christmas morning telling them we were pregnant.
January 2019: We decided to give Clomid one last shot since I responded so much ‘better’ in terms of number of follicles to Clomid. One lead follicle in my right ovary -> not pregnant. I took this pregnancy test on my birthday thinking what a great 35th birthday present after over a year of TTC! The Clomid also caused another round of ovarian cysts as a side effect so back on birth control to quiet the ovaries and let them go away on their own.
February 2019: Ovarian cyst again. Had to sit another month out.
What are the statistics for conceiving at this point?
After four months of monitored cycles on medication, it was time for Fred and I to get realistic about our options and move on to the next step. For reference, here are the statistics Dr. Steward had gone over with us from the beginning. They look pretty depressing, but having two healthy pregnancies under our belt, we were always optimistic that the next month it was going to work. I am gratful to Dr. Steward for never pressuring us to move to the next thing and always letting us take it in stride and work at our own pace.
An average pregnancy rate each month for a normal couple at age 35 is 15%. After TTC for over a year, you are now considered an ‘infertile’ couple. For an infertile couple at age 35, your pregnancy rate drops from 15% to <5% each month.
We started with fertility pills (Clomid / Letrozole) and timed intercourse which increases your chances from 5% to just 10% each month. This is what we did the first four months seeing our fertility doctor (see above). Again, this is a personal choice and you can go at your own pace with these decisions.
Fertility pills (Clomid / Letrozole) and IUI increase your chances of conceiving to 12% and fertility injections and IUI increases your pregnancy rate to 20%. However, with fertility pills the twin rate goes up to 10% and with fertility injections the twin rate goes up to 20%. So it is all a delicate, personal balance to what you feel comfortable with personally.
What were your next steps?
When our ‘Step One’ didn’t work for us, we decided to weigh our options for our ‘Step Two’. Again, everyone makes these decisions based on their personal choices after discussing their unique case with their doctor. I think we were pretty conservative and I am grateful to Dr. Steward who told us the statistics, but ultimately never pressured us and let us go at our own pace.
March 2019: We decided to try fertility pills combined with IUI which would only increase our chances of getting pregnant to 12%, but keep the twins rate down to 10%. Because of my two pre-term labors with the boys, our doctor did not want me to get pregnant with twins with my history. We didn’t get pregnant this month.
April 2019: We decided to give IUI another try, but this time with fertility injections instead of fertility pills. This increases the pregnancy rate to 20% (but also increases the twin rate to 20%). Everything in terms of follicles, uterine lining thickness, etc. looked the best Dr. Steward had ever seen for us this cycle so we were optimistic that this was going to be IT! We didn’t get pregnant this month either. Plus, another month of follicular cysts as a side effect to the injections.
May 2019: Ovarian cyst again. Had to sit another month out.
The Path to IVF for Us

May 2019: While I was on birth control again for the follicular cyst, Fred and I started discussing what was next for us. We had now been TTC for 16 months, 6 of those months were actively TTC with fertility treatments (not including the months we had to sit out due to ovarian cysts). After four failed monitored cycles with fertility medicine and two failed IUIs, we felt like it was time to decide if we were okay moving on with our two precious boys and leaving the dreams of growing our family with another baby behind or was if we were ready to consider IVF. Honestly, this wasn’t something we ever thought we would do since we do have two precious boys, but my heart ached for another baby and Fred being the supportive and loving husband that he is was now willing to fully explore it.
To be completely honest, we struggled with what IVF meant to us from a religious perspective. We are not Catholic, but we are Christians and since we had never been put in this position before, we hadn’t given our views on this enough thought before now. So we made an appointment to talk to our pastor, Dr. Pace at St. Luke’s United Methodist here in Houston. I personally cried the entire hour we met with him. I think the stress of all the failed months of trying finally hit me as I had been relatively patient and optimic before now. I also felt extremely guilty for feeling sad about not conceiving and wanting another baby when I had so much to be thankful for with our two, perfect boys knowing so many others were struggling to conceive for their first child. I am not going to get in to the details of our meeting or the questions we had for Dr. Pace, but I would encourage you if you ever find yourself in the same position to talk to a pastor or a mentor. Fred and I both left the meeting feeling so at peace and on the same page with our decision. That day we decided to move forward with one round of IVF (one egg retrieval). We both agreed if that didn’t work, we would be happy with our sweet family of four and know that we had given it our all.
Can you tell us about your IVF experience?

June 2019: We started the IVF process. For those of you not familiar with IVF, think of it as a two step process. The first step is ‘the retrieval’ which is similar to previous fertility injections I had done with IUI, but the drugs are much stronger and a little more complicated to administer. They require mixing powders and liquids, getting up to six shots a day (depending on your dosage), plus oral medicine and going in to see your doctor typically every other day for blood work and sonogram monitoring leading up to retrieval day. (For reference to anyone going through this, I was up to four vials of Menopur 300 IU, Gonal-F 300 IU, and 0.25 of Cetrotide 0.25 mg before my retrieval.)
For the actual retrieval procedure, you are put under general anesthesia for the doctor to retrieve the eggs from your uterus. I felt all the previous fertility treatments we had done were good ‘practice’ for the big game so to speak. I had become more comfortable with shots and gotten use to all the blood work and monitoring appointments so it wasn’t as much of a shock as it would have been if we had started with IVF.
I also think at now 33 weeks pregnant, time has blocked some of the worst parts from my memory where it doesn’t seem as bad in hindsight. Funny how our memory works isn’t it?! The one tip I have is to take notes or video at your learning appointment with the nurse so when you get home you feel more confident mixing your medicine and administering the shots. I remember coming home and being SO nervous that first day that we would mess something up. When Fred was home he would give me the shots, but due to his travel schedule, there were times I had to give them to myself. (Our pharmacy also provided links to videos on the web that were a lifesaver to watch those first few days.)
The day of the retrieval, we got six eggs, but only four of them were mature. The following day we learned that all four of the mature eggs fertilized. On day 3 we received the update that only two of the four had made it and by days 5-6 both of the two embryos had continued to develop into the blastocysts stage. Most practices also use an embryo scoring system, which includes cell number, cleavage rate, and percentage of fragmentation and symmetry of cells. This is all beyond my understanding, but our lab grades them with the labels ‘good, fair and poor’ in two categories. Our embryos were graded ‘good, fair’ and ‘fair, fair’. We were cautiously optimistic at this point, but we had made it past the first hurdle with two embryos!
Step 2 of IVF is the ‘transfer’ where they transfer the embryo(s) into the uterus and you have the dreaded two week wait before you have your official pregnancy test blood work to find out if the embryo implanted and you are pregnant. This stage of IVF is generally much easier than the first step. There is less medicine leading up to the transfer and the transfer itself is pretty painless (you are not put under this time). The hardest part about this stage (medically speaking) is the progesterone shots. The shot itself isn’t too painful, it is the injection site after the daily shots that gets really tender and swollen. I also had an allergic reaction to the sesame oil in the shot so it became incredibly swollen and itchy at my injection site. Once they switch the oil, it was much easier for me which is a good thing because if you get pregnant, you keep taking the shots until the end of your first trimester! Yes, that’s ~14 weeks of shots when you finally make it to this stage!
July 15th 2019: We made it to transfer day! Our doctor and practice recommend bed rest or taking things light after the transfer so my parents took both the boys to Corsicana for a few days so I could rest at home after the transfer. This was amazing logistically, but also emotionally so Fred and I could just focus on this and know the boys were having fun with their grandparents. I didn’t sleep well the night before the transfer because I was so nervous! Before our procedure, Dr. Steward came in to answer any questions and walk us through the process. At this time they also give you an update on your embryo as they are thawing it before the procedure. Forgive my lack of technical terms and details here because it all seems like a blur, but Dr. Steward told us our embryo had a lot of fragmenting which lowered our pregnancy rate from ~60% to ~50%. Since we only had two embryos, he advised moving forward with a single embryo transfer as planned. Statistically speaking, you don’t want to put all your eggs in one basket (no pun intended) should the transfer not take since we wouldn’t have anything left to work with if we transferred both embryos and neither took. Additionally, he didn’t like the idea of me carrying twins due to my two previous preterm deliveries. So we all hoped and prayed for the best and continued the course. After the procedure, Dr. Steward told us everything went ‘textbook’ and we all prayed for the best as it was now in God’s hands.
The Two Week Wait
On day three post frozen embryo transfer (D3PFET), we left for our family vacation to Telluride. This timing wasn’t planned since we booked our trip earlier in the year with another family, but it turned out to be the best blessing to keep my mind occupied leading up to the ‘official’ pregnancy test. I was very active on the trip with a lot of walking, light hiking (we are talking hikes you can do with a 3 and 5 year old), bike riding, etc. I was diligent to drink SO much water every day to stay hydrated, to limit alcohol and caffeine intake, and to avoid hot baths / hot tubs (which was particularly hard when there are jacuzzis involved), but other than that I was pretty much just living our normal life.
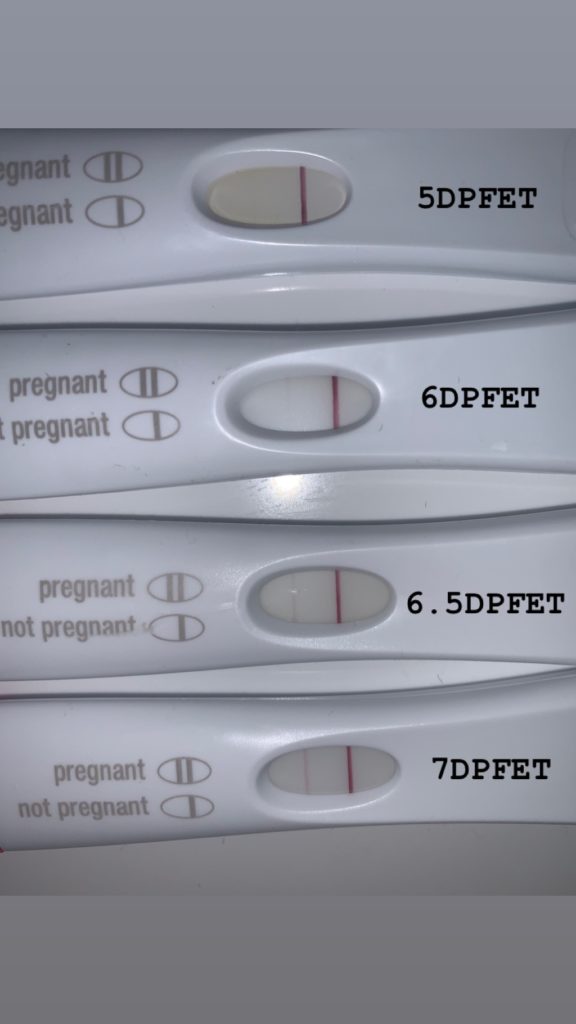
I have zero self control when it comes to waiting to take pregnancy test. I mean if I could have all the money back I spent over the past +20 months of TTC I would be rich! So true to form, I started testing on D5PFET. If you are still reading at this point, you are probably a fellow fertility warrior so I am including a picture of my test each day from day 5-7. On day 7 was the first clear positive. Of course I continued taking test every day until our Dr’s appointment on day 10 PFET where they confirmed I was pregnant when my HCG came back 278.7 mIU/mL!
Did you do anything outside of seeing a fertility doctor?

In addition to seeing Dr. Steward at HFI, I also started seeing a regular acupuncturist at the same time. I followed their supplement recommendations and treatment schedule, but was more lenient on the diet over time. (I wish I could report that I was better in that department, too!) I am listing my instructions from the acupuncturist for your reference below:
Daily Supplements:
- Daily Plant Based Prenatal Vitamin for obvious reasons (I love Ritual, use code ‘Harper’ for 10% off)
- B-Complex for stress
- ProOmega D x 2 in the morning for egg quality
- Ubiquinol (morning and evening) for egg quality
- Royal Jelly x 2 in the morning for egg quality
Diet recommendations specific for my egg quality: Minimize wheat flour and animal dairy, eat 2-3 eggs for breakfast daily, early bedtime and 3L of water daily.
General Diet Recommendations for Infertility:
- Reduce or eliminate alcohol and soft-drinks
- Minimal caffeine, sugar and wheat flour
- Keep a regular rhythm with meals and sleep schedule
- Count 25-50 deep, relaxed breaths daily
- regular dinner should be light and at least 2 hours before bedtime
- Remember the ABC’s of what you can control: Attitude, Breathing and Choices
- Expect positive thoughts and you are more likely to achieve them. 😉
Final Thoughts

I’m finally sharing our story two days after my 36th birthday which is kind of funny to think we ‘planned’ to be done having kids by 34. Though this was not our timing for growing our family, we truly believe everything is His perfect plan and His perfect timing. I am grateful the boys are a little older now and will (hopefully) be more help. I am thankful the boys are both in school now and I am hopeful I will be able to enjoy the newborn snuggles more and cherish even the hard parts of the newborn phase more as we have a better handle on life with two wild boys. I am grateful for the perspective, patience and faith this journey taught us. And I am so EXCITED to meet this little blessing in a few short weeks.
I am happy to answer any questions I may have missed. Feel free to ask them in the comments below or to email me if that makes you feel more comfortable. Please know you are not alone and we are praying for your little miracle to come soon!








Love you and such a special way to share your journey. Even though I walked this with you it really gave me a better insight into your heart and emotional upheavals. Can’t wait for our baby girl❤️
Thank you for sharing ! My husband and I have been on our TTC journey for 19 months. After six IUIs and two pregnancy losses we are moving to IVF and starting at the end of this month. We cannot wait to start our family! Out of curiosity, did you and your husband consider genetic testing ? We are leaning toward trying a fresh transfer but I have never been so torn on a decision in my life.
Xoxo
Justine
Thank you for sharing! My husband and I have been on our TTC journery for 22 months. I am turning 34 this weekend and we are hopeful that we will be able to start our family soon. After 6 IUIs and two pregnancy losses we are starting IVF in March. Out of curiosity, did you consider genetic testing? We have never been more torn on something in our lives! Also, why did you opt for a FET over a fresh transfer?
XOXO
Justine
We are so happy for you!!
We’ve been fighting for 3 tears now,and I’m usually not a crybaby,but “fellow fertility warrior“ made me burst into tears.It’s so hard.I’m happy for every mama out there who wins this thing,and wish you the best of luck.
Did you find out before implantation if it was going to be a girl or boy? We did clomid + iui and now have twin girls!
I so appreciated you sharing your story! I have walked a similar journey with two healthy boys and no trouble conceiving them. My first i had at 30. My second son at 32. I had it all mapped out to have a 3rd at 34 and maybe a 4th at 36. But now TTC for almost 7 years! We miscarried 3 years ago but other than that we have just not been able to conceive and am in my late 30’s now. So I understand all the highs and lows you described and how every month you can hardly hardly wait to check if you are pregnant. You start dreaming and visualizing how this timing really is perfect and yes even how you will break the news to your husband. Even after all these years i still get hopeful every month!! My husband and I both checked out as normal and just have “unexplained infertility”. Though it is a difficult journey to walk, I am comforted that God’s is sovereign and knows what is best for our family. It is helpful to hear other’s stories. Thank you for sharing yours! I can’t wait to “meet” your baby girl! I love your blog and your house/ fashion so much and have followed for several years. Blessings to you and yours 💙
I just read your blog post. A very familiar story to me too. We tried for 4 years to have a baby. In the end, IVF was our decision and with that came 2 baby girls. Caroline and Cate are 13 now and are the best of friends. We laugh, cry and love. My relationship with my two 13 year olds is nothing I imagined a relationship would be with teenagers. They are so fun!
On another note, infertility is something you would not wish on your worst enemy. It’s not natural, no matter what stage you are in your family. One thing I always tell people who were in your situation of already having children. Never feel guilty for doing what you need to do to complete your family. We all have different dreams of what we want our family to look like. Yours are Fred’s was 3.
I wish you the best with your baby girl. It truly is SO MUCH FUN dressing them. Until it’s not! Haha!
Loved reading your story. My favorite part is when you described each month how you imagined telling your husband or your family, because for anyone that has struggled to conceive this is such a reality. My husband and I similarly had no difficulty TTC our first daughter. We tried for a year the second time around and I ended up with a positive pregnancy test the morning I was scheduled to go in for a laparoscopy. I am due with our second baby girl any day now. It is true that the Lord’s timing and plan are perfect but the waiting is SO hard.
Heartiest congratulations Caroline! Long time reader of yours here. I am a mom of two cute girls (both conceived easily) but I read every word of our story just to remind myself how truly grateful we should be. All the best for your beautiful family!
http://www.docdivatraveller.com
A detailed, fully customized sleep plan This will be prepared for you after our consultation and after the nights stay so you have your own personalized plan to help guide you through the upcoming nights.
Thank you for sharing your story!! My husband and I tried for a year before conceiving (twins!) with IUI and Clomid. This was our first attempt at getting pregnant, and the disappointment each month was brutal. I would also get this hope each month (like your Germany pregnancy test or birthday pregnancy test) just to be disappointed again. I think it’s very brave of you to share your story with the world, and I hope your story helps all the other women out there battling unexplained fertility! I, for one, am very excited to follow along your pregnancy journey as I embark on my own <3
Wishing you a smooth pregnancy and delivery!
All I can say…I’m very happy for you & Fred- I have been following you since your NY days- can’t wait for posts of your beautiful baby girl- God bless.
Do you have any plans for the other frozen embryo?
Good know about you .